Prioritizing the Backlog of Routine Referrals to Optimize Specialist Capacity
The Challenge of Prioritizing Referrals and Specialist Capacity
Care Continuity partnered with a regional health system with a growing footprint in multiple markets across two states. The organization had built a medical group network of more that 900 physicians including PCP and specialist providers - along with a Clinically Integrated Network (CIN) of more than 2,000 affiliated providers. To manage specialist referrals the health system had recently centralized its Patient Access team, and also rolled out new self-service scheduling tools in some markets – but they still struggled to match the right patients with the priority specialist appointment slots.

Smart Segmentation of the Referral Backlog
The health system had basic work queues in their EHR for referral scheduling, but more than 90% were marked as “routine” and followed a “first-in-first-out” prioritization based on referral date. Partnering with Care Continuity, they implemented a referral scoring model for the new Patient Access Center to prioritize the rolling backlog of more than 50,000 specialist referrals. This enabled navigation staff to work smarter and schedule more high-priority patients with in-network specialists - reducing network leakage and improving downstream revenue
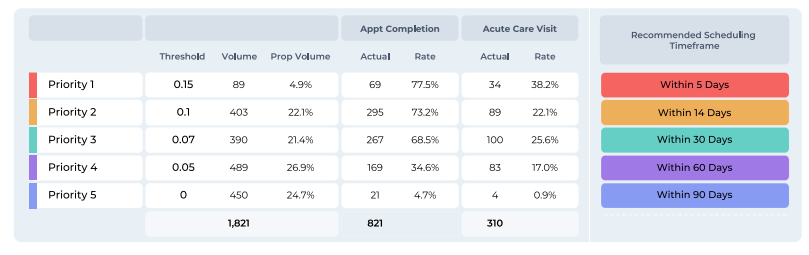
Prioritizing Downstream Procedures, Avoiding Acute Events and No Shows
The health system optimized their referral scoring model to predict three key outcomes. First they identified patients most likely to have a downstream procedure that could be captured by the health system network in the next 120 days. They also looked at clinical risks, predicting which patients were likely to have an unplanned acute event resulting in an ED visit or IP stay. Finally they modeled the likelihood of appointment no-shows, to ensure specialist schedules were optimized. For each specialty, the health system weighted these factors differently based on the unique challenges for that service line.
Impacting The Bottom Line
The health system monitored referral patterns for every PCP and Specialist practice and measured in-network completion rates for high-priority patient referrals. To better understand their own provider network, they also tracked appointment wait times and no-show rates for every specialist office. By focusing on high-value referrals, the system saw growth in downstream utilization rates and realigned their provider network relationships to reduce revenue leakage to competitors in each market. Ultimately, their owned medical group saw a better mix of high-priority patients and optimized their limited appointment capacity.

Recent Stories
Ready to close the loop on follow-up care? Let’s connect.

